Context
Pomona Valley Hospital Medical Center (PVHMC) is a 53-bed level 3B NICU. The NICU receives referrals from the labor and delivery department with approximately 5000 births annually. The NICU admission rate is approximately 12% of all live births. Well Infants with birth gestational age of 35 weeks and higher are routinely admitted to normal newborn nursery unless they become sick either at birth or later. Infants with complex heart conditions and need for extracorporeal membrane oxygenation (ECMO) are referred to the nearby tertiary center. SSC recommends that infants suspected of sepsis receive their first antibiotic dose within 60 min of being ordered. We obtained our data by manual review of patient charts, the medication administration record (MAR) and the time of physician orders for antibiotics on all patients. Our baseline data showed that only 32.7% of prescribed antibiotics were given within 60 min of the order being placed. During the same time period the average time to administer the first dose of antibiotics was 93.3 min. In October 2020, after consultation with the NICU antibiotic stewardship program(ASP), we assembled a multidisciplinary team of stakeholders that included neonatologists, nurses, pharmacists and infection prevention staff.
During the baseline year 2020, there were six hundred and seventy-five (675) admissions to the NICU. Three hundred seventy (370 or 54.8%) of these infants were prescribed antibiotics at least once during the NICU stay. During the three-year duration of the project (January 2021 to December 2023), two thousand two hundred and one (2201) patients were admitted to the NICU. Of these, one thousand and ninety-four (1094 or 49.7%) of these patients were prescribed antibiotics at least once during their NICU stay. We created a fishbone diagram (Fig. 1), developed an AIM statement and designed a key driver diagram to facilitate change for our project (Fig. 2).

Illustrating root causes of delays in antibiotic administration, informed by Surviving Sepsis Campaign (SSC) principles and categorized into ordering process, shared staff mental model, measurement, and delivery system.
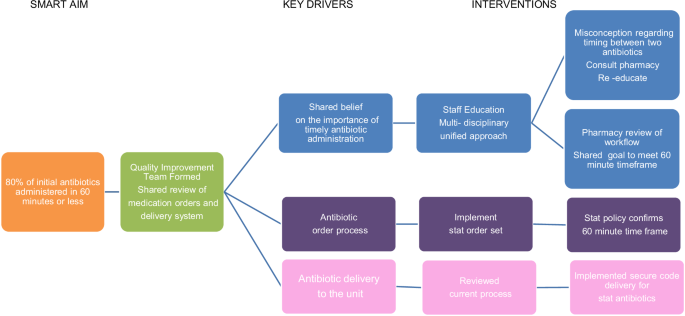
Illustrating the key drivers and interventions to achieve timely antibiotic administration in the NICU.
Interventions
Staff Education, Quarter 1, 2021 (PDSA 1)
We engaged the NICU staff and the pharmacy department and shared our project AIM with them via email. An educational program was developed and posted on the hospital’s learning management system (LMS). The staff members were expected to complete the education module in a 30- day period. The module included education on results of practice audit, sepsis risk factors, the SSC, goals for timely administration and the performance improvement plan. It also required a test at the end of the module to assess staff knowledge and retention of the educated material. A 100% compliance with the module was obtained at the end of the 30 day period.
Staff re-education and shared understanding of the antibiotic administration
A review of the data for first quarter 2021 revealed modest improvement with timely administration of the antibiotics increasing to 53.5% (Fig. 3) and an average time of administration noted at 72.9 min (Fig. 4) after being ordered. We reached out to staff members in April 2021 to identify barriers they may have encountered during the administration of antibiotics. The staff feedback identified a shared belief among the staff members that any two antibiotics needed a 60-min interval in between the two antibiotics. Our practice is to order two antibiotics for suspected sepsis and to give both within 60 min of ordering. There was a misconception that originated from a previous practice of separating the antibiotic administration while obtaining drug levels. Although this was not relevant to our current project, that misconception led to the practice of separating any two antibiotics, resulting in delayed administration. Delays in getting the antibiotics from the pharmacy was also identified. Although the hospital had an existing policy of what a stat order means, not all antibiotics were being ordered stat. Therefore, pharmacy was not compelled to deliver an antibiotic within 60 min. Lack of a dedicated NICU pharmacist at night further delayed antibiotic delivery. We concluded that these two factors required further interventions. A decision was made to re-educate staff members. An education module was again developed and sent to staff via LMS portal. This education module included reinforcement for timely administration and correcting the misconception regarding the safety of back-to-back administration of the first stat doses of antibiotics. The pharmacy conducted an internal review of their processes in order to improve workflow and agreed to make the antibiotic dosages available within 30 min of being ordered. With this change we anticipated that the staff could administer it within 30 min after having received the medication from pharmacy. Review of data after another 6 months revealed modest improvement. The percentage of infants receiving the first dose of antibiotics within 60 min of ordering improved to 56.9% (Fig. 3) and the average time interval improved to 62 min (Fig. 4). However, these outcome numbers were still below our stated AIM.

Control chart illustrating the percentage of patients per quarter (Q) receiving antibiotics within 60 min over time. The chart includes the upper control limits (UCL) and lower control limit (LCL) to indicate process variation. PDSA (Plan-Do-Study-Act) cycles 1, 2 and 3 are indicated, showing the impact of iterative quality improvement interventions on timely antibiotic delivery.

Control chart showing the average time to antibiotic administration in minutes by quarter (Q). Upper and lower control limits (UCL and LCL) indicate process variation around the mean. PDSA (Plan-Do-Study-Act) cycles 1, 2, and 3 are indicated to show points of intervention during the study period.
2022: Creation of an order set for stat first dose of antibiotics. (PDSA 2)
Initial review of the literature revealed that most institutions were developing stat order sets for administration of antibiotic dosages. The pharmacy department created a list of commonly used antibiotics in NICU. In January 2022, with the help of the Information Technology (IT) department, we developed stat order sets for the commonly used antibiotics that included Ampicillin, Gentamicin, Cefepime, Penicillin G, Ceftazidime, Meropenem, Oxacillin, Vancomycin, Piperacillin-Tazobactam, Ampicillin-Sulbactam, Cefoxitin and Ceftaroline.
Per our institution’s stat dose policy, any medication ordered stat must be administered within 60 min of being ordered. This enhanced the team focus on optimization, allowing the ordered antibiotic to be available within 30 min to the NICU for administration to the patient. Review of data after 6 months showed inconsistent improvement in primary outcome to 59% (Fig. 3) while the secondary outcome remained essentially unchanged at 61 min (Fig. 4).
July 2022: Implementation of secure code delivery for antibiotics (PDSA 3)
We had expected significant improvement with the order set changes but the results were not satisfactory and did not meet the stated goals. We reviewed our medication delivery system to identify the source of the problem. According to the existing delivery system at that time, the pharmacy would prepare the stat antibiotic dose and send it via the tube delivery system to the NICU. Upon arrival to the NICU the medication was placed in the medication tray. The nurse would then have to pick up the medication and bring it to the bedside for administration. By this system it was not certain when the nurse would pick up the medication, hence resulting in unpredictable time between arrival and delivery to the bedside. We amended this process in order to make it more efficient. The new proposed system included a secure code for delivery of stat antibiotics. Any stat antibiotic delivered to the NICU via the internal tube delivery system rings an alarm, alerting the staff in the immediate vicinity to pick up the antibiotic and deliver it to the bedside nurse for administration.
This system eliminated any lost time from arrival to the delivery at bedside. This system also allowed us to document the time when the medication was prepared and dispatched by pharmacy, the time it arrived in the NICU and the time it was actually administered to the intended patient. In the three months following the implementation of the secure code delivery, the percentage of infants receiving the stat dose of antibiotics within 60 min improved to 88% (Fig. 3). The average time of the administered antibiotic improved to 43 min from the ordering time (Fig. 4). These results were sustained for 2 years after the implementation of the secure code delivery system.
Measures and analysis
Primary outcome
was defined as the percent of infants receiving their stat first dose of antibiotics within 60 min of having been ordered.
Secondary outcome
was defined as the average time from ordering to administration of the first stat dose of antibiotics.
Balancing measures
To ensure no unintended consequences were introduced, we monitored error rates as a balancing measure, including ordering, pharmacy and administration related errors. No errors were identified during the study period. Our neonatal mortality rate per 1000 admissions was 11.9% during the baseline year and after some variation, decreased to 8.2% in 2023 and remained stable during the length of the project. Although not statistically significant, a downward trend led us to believe that there was not an unintended adverse clinical outcome.
We used 12 months of data from January 2020 to December 2020 to establish a baseline and 42 months of data from January 2021 to June 2024 to demonstrate sustainability. Statistical control charts (P Charts) were used for plotting the primary and the secondary outcomes on a quarterly basis. Upper and lower control limits were set at 3 standard deviations above or below the process mean. We used standard rules for common cause variation and special cause variation for healthcare. All data was collected from the NICU EMR. Periodic review of the data was conducted at the Quality Improvement committee meetings.
Ethical considerations
The project was conducted in accordance with “Protecting Human Research Participants” guidelines. Confidentiality of the participants was maintained by anonymizing the data and securely storing it. The Institutional Review Board at PVHMC provided a waiver, ensuring that all ethical considerations were reviewed and approved.






