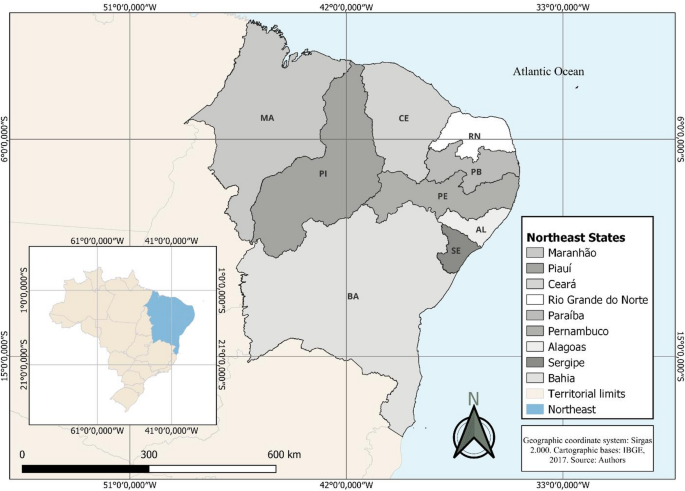
Epidemiological characteristics of VL in northeastern Brazil (2007–2022)
Between 2007 and 2022, a total of 143,414 cases of VL were reported in Brazil, comprising 54,003 confirmed cases, with the northeastern region accounting for 28,920 of these cases (Table 1). The analysis revealed a significant predominance of cases among men (66.0%), children under 10 years old (44.6%), and individuals of mixed race (81.4%). The most frequently reported symptoms included fever (89.9%), weakness (76.6%), spleen enlargement (76.3%), pallor (72.1%), weight loss (69.4%), and liver enlargement (64.4%).
New cases accounted for approximately 93% of the case types, with most transmissions occurring at the municipality of residence (83.3%). Laboratory tests were performed for 83.3% of cases; however, over half of the patients did not undergo specific parasitological or immunological tests for VL. Despite inconsistencies in data reporting in the SINAN notification form, 78.8% of patients received treatment and subsequently recovered. Sample sizes varied due to missing or undeclared information, and only epidemiologically confirmed cases from the relevant years were included in this analysis.
Spatial distribution of VL incidence
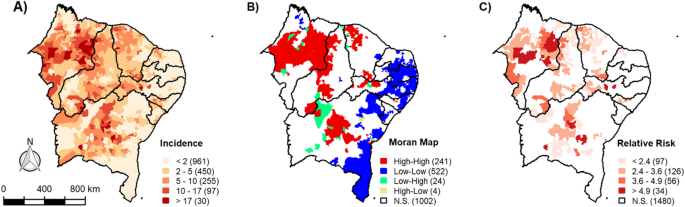
Figure 1 illustrates the spatial distribution of VL incidence across northeastern Brazil from 2007 to 2022. Figure 1A highlights regions with the highest incidence rates (above 17.0 per 100,000 inhabitants), primarily concentrated in the states of Maranhão, Bahia, Piauí, and Ceará, which are the most critical areas for transmission of VL. The univariate spatial analysis confirmed a positive spatial autocorrelation for VL incidence (Global Moran’s I = 0.47; p < 0.001), further validated by the Bayesian Index (I = 0.61; p < 0.001), suggesting significant spatial patterns of dependency among neighboring municipalities. Notably, VL cases were reported in nearly all municipalities throughout northeastern Brazil.
Spatial distribution of visceral leishmaniasis (VL) incidence in northeastern Brazil from 2007 to 2022. (A) VL incidence rate per 100,000 inhabitants, highlighting a higher concentration of cases in the northern and central regions of the northeastern. (B) Local spatial autocorrelation map (Local Moran’s I), identifying significant spatial clusters. (C) Relative risk map, highlighting areas with a higher risk of VL transmission compared to other regions. This figure was created using the R (version 4.4.1) programming language through the RStudio environment. The shapefiles were obtained from the geobr package (https://www.r-project.org/).
Local Moran’s I (Fig. 1B) reveals spatial clusters of VL incidence, identifying 241 municipalities as High/High, which indicates significantly high VL rates. Maranhão, Piauí, Bahia, and Ceará represent most of these municipalities. Other states, such as Pernambuco and Alagoas, exhibit isolated municipalities with similar spatial patterns. Additionally, coastal regions of northeastern Brazil show Low/Low clusters, indicating areas with lower VL incidence, although they remain endemic for the disease. In the context of VL incidence, the LISA quadrants offer meaningful spatial interpretations: Q1 (High/High) indicates transmission hotspots, where high incidence is surrounded by similarly high values; Q2 (Low/High) may suggest areas at risk of expansion; Q3 (Low/Low) reflects regions with consistently low incidence; and Q4 (High/Low) points to isolated high-incidence areas, possibly representing emerging clusters or localized outbreaks.
Highlighted areas of relative risk (RR) for VL transmission (Fig. 1C) identified 34 municipalities with an RR greater than 4.9, especially in Maranhão, Bahia, and Pernambuco. Municipalities with moderate RR (3.4 to 4.9) are located in Ceará and Piauí, while other states display lower RR values (RR < 3.4).
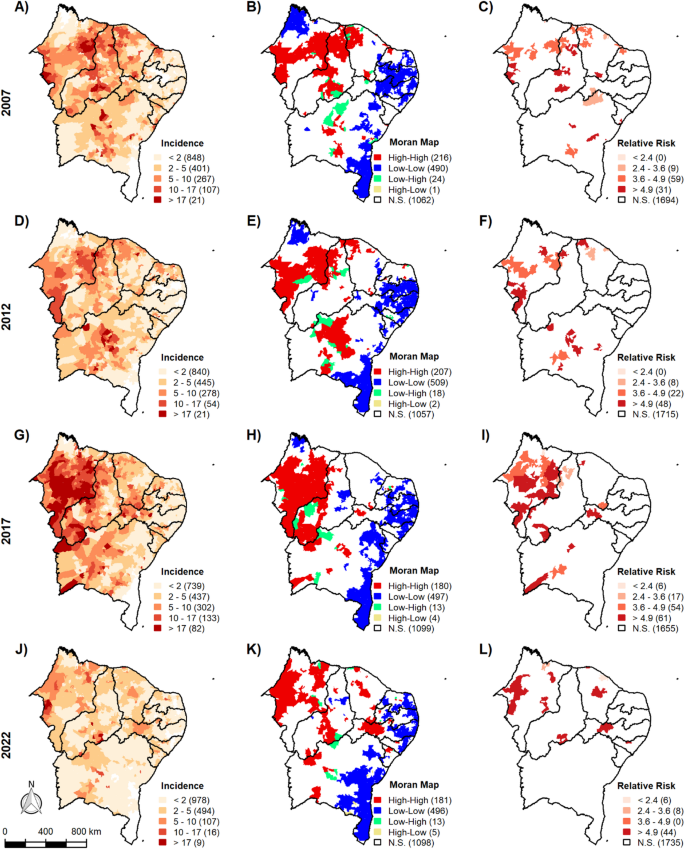
In 2007 (Fig. 2A–C), most municipalities presented low incidence rates (< 2 cases per 100,000 inhabitants), with few clusters of high incidences. The Moran map identified 216 municipalities classified as High-High and 490 as Low-Low, with a predominance of non-significant areas (N.S.). The relative risk values were also mostly concentrated in the non-significant category (n = 1,694), with only a few areas showing risk values above 4.9. In 2012 (Fig. 2D–F), an increase in incidence magnitude was observed in several areas, with growth in the number of municipalities within the intermediate incidence strata (5–10 and 10–17). The number of municipalities in High-High and Low-Low clusters remained high (207 and 508, respectively), with a reduction in N.S. areas, suggesting a stronger spatial structure of the disease. Relative risk maps showed a slight expansion of areas with values between 3.6 and 4.9 and > 4.9, especially in the northern and northwestern parts of the region.
Spatial distribution of the incidence of visceral leishmaniasis (VL) in northeastern Brazil in the years 2007, 2012, 2017 and 2022. Maps A, D, G and J show the VL incidence rate per 100,000 inhabitants. Maps B, E, H and K show the local spatial autocorrelation (Local Moran’s I). Maps C, F, I and L show the relative risk. This figure was created using the R (version 4.4.1) programming language through the RStudio environment. The shapefiles were obtained from the geobr package (https://www.r-project.org/).
The year 2017 (Fig. 2G–I) represented the peak of both spatial aggregation and disease magnitude. Incidence rates were markedly higher, with extensive areas surpassing 10 cases per 100,000 inhabitants, mainly concentrated in Maranhão, south-central Piauí, and western Bahia. Spatial clusters were more evident, with 180 municipalities classified as High-High and 497 as Low-Low. Relative risk values also increased substantially, with 94 municipalities showing RR > 4.9 and 54 between 3.6 and 4.9, indicating high-risk regions consistent with Moran clusters. In 2022 (Fig. 2J–L), a general reduction in incidence and spatial clustering was observed. Although some high-incidence areas persisted, particularly in Maranhão, there was a decline in the highest incidence values and an expansion of areas with incidence between 2 and 5 cases per 100,000 inhabitants. Nevertheless, Moran maps still showed 181 municipalities classified as High-High and 496 as Low-Low, with most areas remaining statistically significant, suggesting that although the magnitude of incidence decreased, the spatial structure of the disease remains present.
The Moran’s I values for crude incidence data increased from 0.09 in 2007 to 0.19 in 2012 and 0.27 in 2017, followed by a reduction to 0.13 in 2022. The values obtained using the empirical Bayesian estimator also showed an upward trend from 0.45 in 2007 to 0.56 in 2012 and 0.61 in 2017, with a subsequent decrease to 0.56 in 2022.
Association between VL and environmental factors
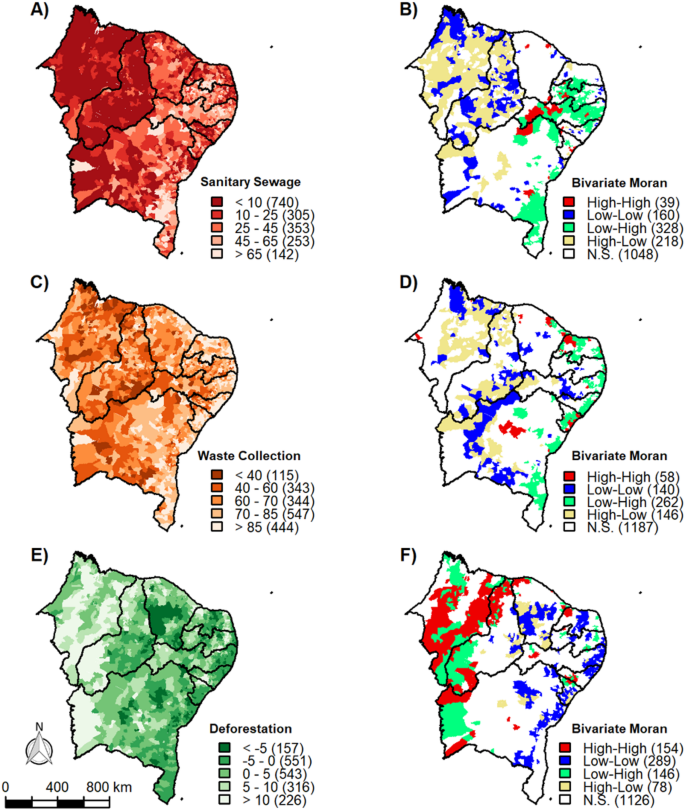
The Global Bivariate Moran’s Index indicated a statistically significant spatial correlation between VL incidence and sanitation (Moran’s Index: −0.31; p < 0.001), waste collection (Moran’s Index: −0.18; p < 0.001), and deforestation (Moran’s Index: 0.20; p < 0.001). Figure 3A and B illustrate the association between sanitation and VL incidence. High VL incidence correlates with inadequate sanitation services in 218 municipalities, predominantly in Maranhão, Piauí, and western Bahia. In contrast, municipalities with higher sanitation coverage, associated with low VL incidence, were located mainly in Pernambuco, Paraíba, and coastal Bahia.
Spatial distribution of environmental factors and their spatial association with visceral leishmaniasis (VL) incidence in the municipalities of northeastern Brazil. Maps A, C, and E show the distribution of sanitary sewage coverage (%), waste collection coverage (%), and cumulative deforested area (hectares), respectively. Maps B, D, and F present the bivariate spatial autocorrelation analysis (bivariate LISA — Moran’s I) between each environmental factor and VL incidence from 2007 to 2022. This figure was created using the R (version 4.4.1) programming language through the RStudio environment. The shapefiles were obtained from the geobr package (https://www.r-project.org/).
Regarding waste collection and VL incidence (Fig. 3C and D), municipalities with low VL incidence but adequate waste collection are primarily found in Pernambuco, Sergipe, Rio Grande do Norte, and Bahia. Conversely, municipalities with high VL incidence and inadequate waste collection services (High/Low) are mainly located in Maranhão and Piauí.
Figures 3E and F illustrate the association between deforestation and VL. A significant positive correlation (High/High) was observed in 154 municipalities, especially in Maranhão and Piauí. Municipalities with low VL incidence and minimal deforestation (Low/Low) were primarily located in Pernambuco and Bahia.
These findings indicate that Maranhão, Piauí, and Bahia face the most critical environmental and epidemiological challenges in the region. In the other states, both incidence and environmental factors maintain a moderate to low status.
Temporal trend of VL incidence.
The overall trend indicates a slight decrease in incidence (AAPC = −0.69%; p < 0.001). While the disease demonstrated a consistent pattern during certain periods, the incidence rate declined from 3.89 per 100,000 inhabitants in 2007 to 3.49 per 100,000 inhabitants in 2022 (Fig. 4).