Patient characteristics
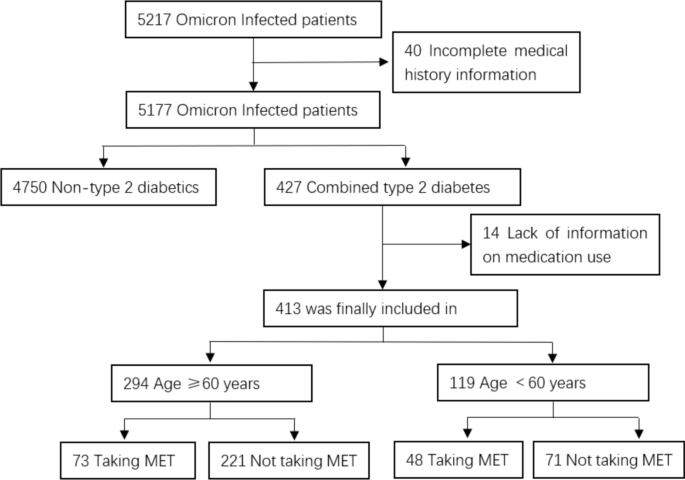
A total of 413 patients with type 2 diabetes melitus (TDM) with a mean age of 66.3 ± 13.9 years were included in this study from a cohort of 5217 cases infected with COVID-19 (Fig. 1). Of these, 287 (69.5%) had at least one comorbidity, including coronary heart disease in 79 (19.1%) cases, hypertension in 210 (50.8%) cases, stroke in 65 (15.7%) cases, chronic kidney disease in 41 (9.9%) cases, chronic lung disease in 7 (1.7%) cases, malignancy in 24 (5.8%) cases, and immunodeficiency in 14 (3.4%) cases. 150 (36.3%) cases of patients have received at least one dose of COVID-19 vaccine. Prior to admission, 121 (29.3%) patients were taking MET, 34 were taking sulfonylureas, 13 were taking gliptins, 10 were taking insulin sensitizers, 55 were taking alpha-glucosidase inhibitors, 27 were taking DPP-4 inhibitors, 38 were taking SGLT-2 inhibitors, 101 were using insulin, and 25 were not using any antidiabetic medication or had been using medication for less than 3 months. There were no significant differences in age, sex, BMI, comorbidity rates, or vaccine doses between patients who received MET and those who did not (Table 1).
Comparison of laboratory results between diabetic patients receiving and not receiving MET treatment
According to the experimental results in Table 2, there were no statistically significant differences in eGFR, Glucose, ALT, Albumin, WBC, Haemoglobin, PLT, PCT, HbA1c, Fibrinogen, cTnI, and BNP levels between diabetic patients receiving and not receiving MET treatment on admission. This means that there were no significant differences in these laboratory results between diabetic patients receiving and not receiving MET therapies.
Comparison of clinical outcomes between diabetic patients receiving and not receiving MET treatment
Among the 413 patients with type 2 diabetes, 126 (30.5%) had pulmonary infiltrates on imaging. Of these, 27 received MET treatment, 18 (4.4%) were classified as severe or critical on admission and 9 (2.2%) cases progressing to severe or critical during hospitalization. Of all severe or critical cases, 2 received MET treatment and all were admitted to the ICU. The mean length of hospital stay for all COVID-19 infected patients with type 2 diabetes was 13.8 ± 7.7 days.
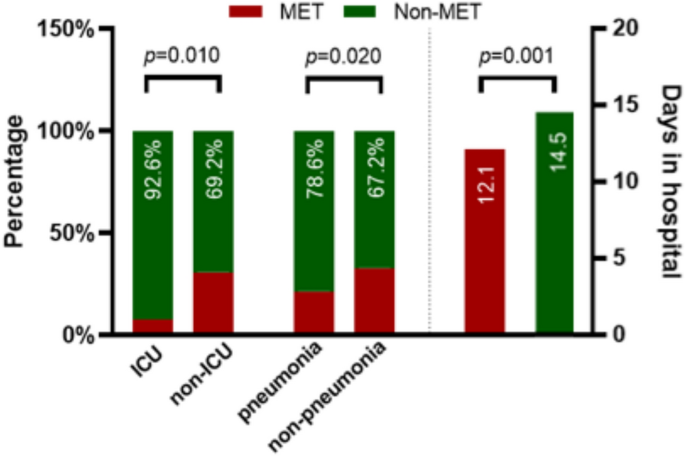
Compared with those who received MET treatment, the proportion of patients admitted to the ICU was significantly higher in those who did not receive MET treatment (69.2% vs. 92.6%, p = 0.010). Similarly, the proportion of patients with pneumonia was significantly higher in those who did not receive MET treatment than in those who did not have pneumonia (67.2% vs. 78.6%, p = 0.020). In addition, patients who received MET treatment had a shorter length of hospital stay than for those who did not receive MET treatment (14.5 ± 8.2 days vs. 12.1 ± 5.9 days, p = 0.001) (Fig. 2).
Comparison between elderly and non-elderly patients receiving and not receiving MET treatment
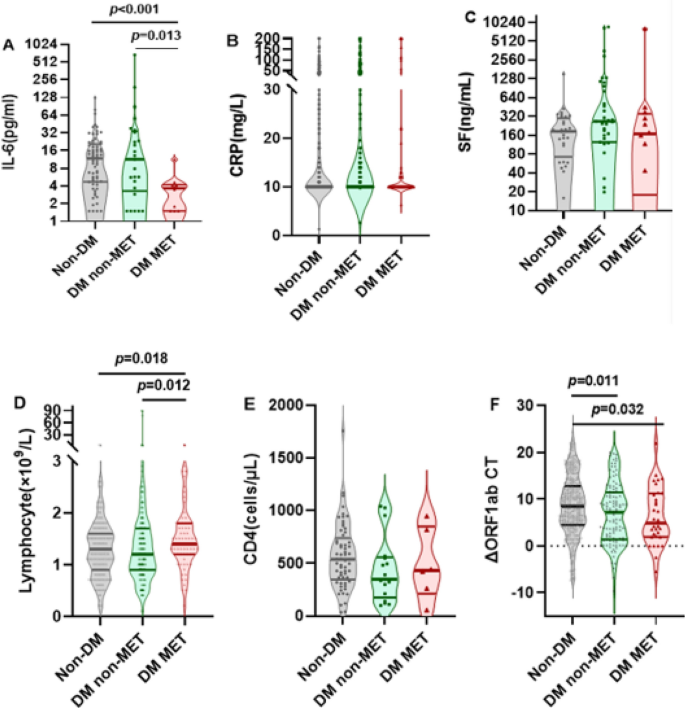
Among patients over 60 years of age (defined as elderly), the proportion of ICU admissions was significantly lower in MET recipients (2.7% vs. 10.4%, p = 0.042), and the length of hospital stay was significantly shorter (12.1 ± 5.5 days vs. 14.9 ± 8.8 days, p = 0.001) (supplementary Table 1). Figure 3 (A-F) demonstrates the differences in levels of inflammation and immune markers between subgroups. The MET-treated patients had significantly lower levels of IL-6 (IQR, 11.4 pg/ml vs. 3.7 pg/ml, p = 0.013; 11.8 pg/ml vs. 3.7 pg/ml, p < 0.001) as compared to the non-diabetic patients of the COVID cohort and those who did not receive MET (Fig. 3A). MET-treated individuals had significantly higher levels of lymphocytes as compared to non-diabetic patients (IQR, 1.3 × 109/L vs. 1.4 × 109/L, p = 0.018) and to those who did not receive MET (IQR, 1.2 × 109/L vs. 1.4 × 109/L, p = 0.012) (Fig. 3D). Compared to non-diabetic patients, both MET-treated individuals and those who did not receive MET had significantly reduced ΔORF1ab CT values (IQR,8.5 vs. 7.2, p = 0.011; 8.5 vs. 4.9, p = 0.032)(Fig. 3F).
Comparison of levels of inflammatory and immune markers between different groups of infected elderly patients (≥ 60 years). Shown are the level of IL-6 (Panel A), CRP (Panel B) and SF (Panel C), the number of lymphocytes (Panel D) and CD4 + cells (Panel E) and the ΔORF1ab CT level (Panel F) in indicated elderly patients (≥ 60 years). Data were analyzed with Mann Whitney test and shown in quartile. Non-DM: Non-type 2 diabetes mellitus group; DM non-MET: Type 2 diabetes mellitus group without MET; DM MET: Type 2 diabetes mellitus group with MET. IL-6,interleukin-6; CRP, c-reactive protein; SF, serum ferritin; ΔORF1ab CT,ORF1ab CT 1 week after admission—ORF1ab CT at admission.
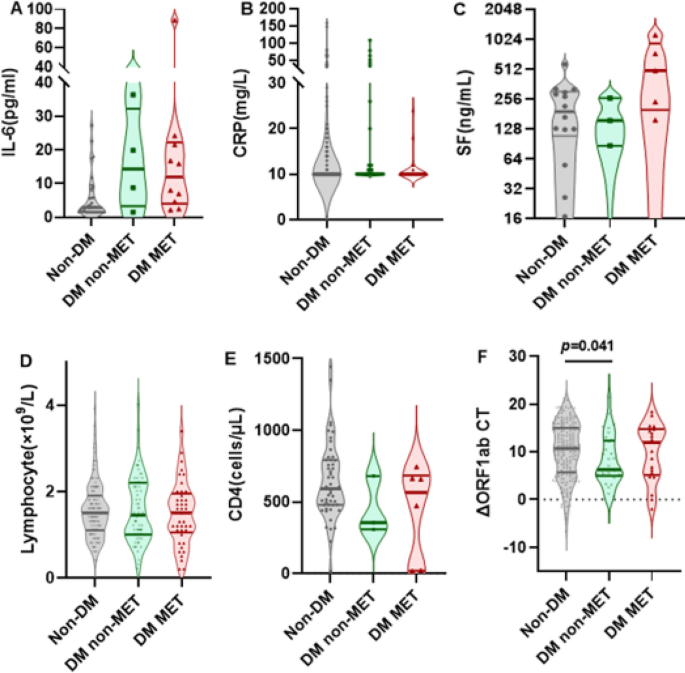
In contrast, for the patients under 60 years of age (defined as non-elderly), there were no significant differences in the risk of ICU admission, pneumonia, and length of hospital stay between MET-treated and non-treated patients (supplementary Table 2). In agreement with this result, none of the inflammation and immunological markers showed significant differences between the MET-treated and non-treated diabetic patients (Fig. 4A–F). Only as compared to non-diabetic individuals, the patients who did not receive MET had significantly increased viral clearance (ΔORF1ab CT, IQR,10.6 vs. 6.3, p = 0.041) (Fig. 4F).
Comparison of levels of inflammatory and immune markers between different groups of infected non-elderly patients (< 60 years). Shown are the level of IL-6 (Panel A), CRP (Panel B) and SF (Panel C), the number of lymphocytes (Panel D) and CD4 + cells (Panel E) and the ΔORF1ab CT level (Panel F) in indicated no-elderly patients (< 60 years). Data were analyzed with Mann Whitney test and shown in quartile. Non-DM: Non-type 2 diabetes mellitus group; DM non-MET: Type 2 diabetes mellitus group without MET; DM MET: Type 2 diabetes mellitus group with MET. IL-6,interleukin-6; CRP, c-reactive protein;SF, serum ferritin; ORF1ab CT: the cycle threshold (Ct) values for amplification of ORF1ab (the expression of the open reading frames 1ab, ORF1ab) from individuals infected with Omicron; ΔORF1ab CT,ORF1ab CT 1 week after admission—ORF1ab CT at admission.
To investigate the possibility that the decrease of inflammatory markers in the elderly patients treated with MET might be due to a slight age and glucose effect, as age and glucose were mildly decreased in the group of receiving MET treatment although not statistically significant (Supplementary Tab1), we analyzed the correlation between IL-6, CRP, SF, lymphocytes, CD4, ΔORF1ab CT and age or glucose. Only ΔORF1ab CT was correlated to age and glucose (Supplementary Table 3), which is consistent with the results that MET treatment did not significantly ameliorate the level of ΔORF1ab CT, and the diabetes patients have a lower ΔORF1ab CT than non-diabetes COVID-19 patients. Moreover, a scatter plot analysis did not reveal a correlation between age, glucose and inflammatory markers in elderly patients (Supplementary Fig. 1). Therefore, we conclude that the beneficial effect of MET on elderly patients is dependent on inflammatory inhibition but independent on age and glucose.