Registry
Between February 2023 and February 2024, 239 patients were eligible for inclusion. 5 patients were excluded because they never started HBOT due to private circumstances, and 2 patients did not provide informed consent. Therefore, 232 patients were included in the final analysis. Of the 232 patients, 187 patients were treated at Eurocept Clinics (Amersfoort, Arnhem, Geldrop, Hoogeveen, Rotterdam and Waalwijk) and 45 patients at the Hyperbaric Medical Center in Rijswijk. The response rate on the primary outcome (SF-36) was 95% at baseline, 84% directly after HBO and 80% at 3-month follow up.
PROMS collection
Unfortunately, due to logistical challenges – particularly at one participating center that was less experienced with follow-up procedures – a substantial portion of the data at the 20 sessions time point was not collected and was lost to follow-up. As a result, these results are not included in the main analysis. However, the data 20 sessions time point (SF-36, EQ-5D, and Long COVID questionnaire) is provided in the appendix (Appendix Tables A, B and D).
Baseline characteristics
Baseline characteristics are presented in Table 1. The median age of patients at the start of the treatment was 42 years (IQR 31–51). Most patients were female (70%) and never-smokers (76%), with only 2% patients being active smokers at the start of treatment. 118 patients had no documented medical history. Of the reported history items in the remaining 114 patients, mental complaints (12%), asthma (11%), irritable bowel syndrome (7.3%), hypertension (4.7%) and other cardiovascular disease (4.7%) were most frequently reported. Most COVID infections that lead to long COVID were confirmed by PCR (71%) or antigen testing (15%). A minority of patients (3%) had been hospitalized for their COVID infection, with none being admitted to the intensive care unit. Patients had long-term complaints before starting HBOT with a median 20 months (IQR 14–30) between SARS-CoV-2 infection and start of HBOT.
HBOT sessions
Patients were treated with a median of 40 sessions (IQR 40–46). 15 (6%) patients terminated their treatment before 37 sessions. Reasons for early termination of the treatment were: HBOT was too exhausting with worsening of fatigue or other long COVID symptoms (10 patients), anxiety or claustrophobia during HBOT (2 patients), no treatment effect (1 patient), an unrelated illness (1 patient), and private circumstances (1 patient).
54 patients received 48 sessions or more. 42 patients because of a (subjective) late response with the wish to extend the treatment, and 12 patients because of inadequate dosing in the beginning of treatment due to interruptions of the treatment schedule (e.g. due to illness).
Primary outcome: SF-36 questionnaire
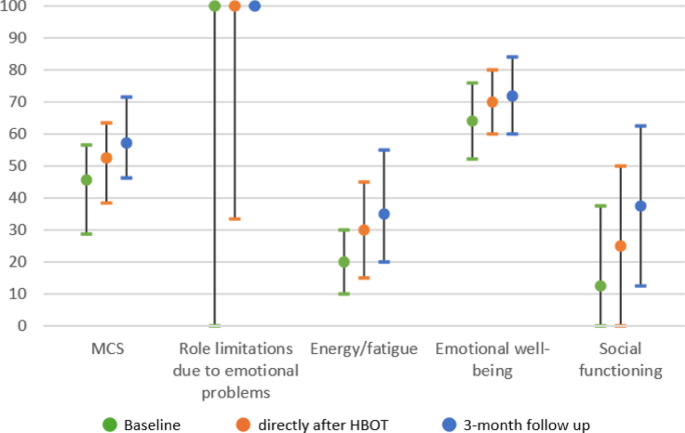
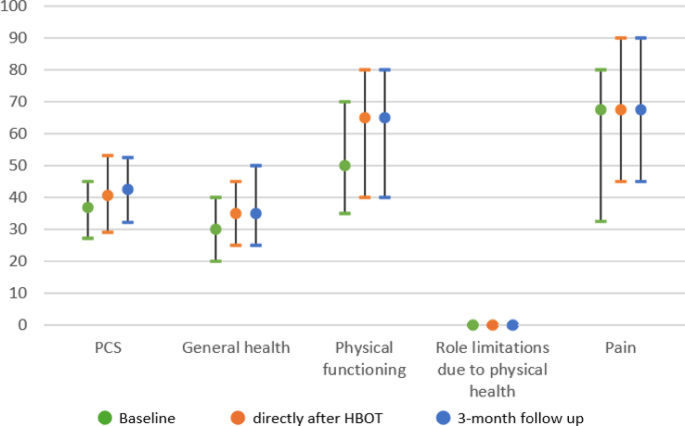
The median MCS of the SF-36 questionnaire improved from 45.5 (IQR 28.7–56.6) at baseline to 57.0 (IQR 46.2–71.5) at 3-month follow up. For the PCS, these scores were 36.9 (IQR 27.2–45.0), and 42.5 (IQR 32.2–52.5), respectively. The Wilcoxon Signed-Rank Test indicated a statistically significant change in median MCS and PCS from baseline to 3 months Z= −7.11, p < 0.001 and Z= −4.53, p < 0.001, respectively. Subdomains that showed the largest increase in score were energy/fatigue, social functioning, emotional well-being and physical functioning (Table 2; Figs.1 and 2).
SF-36 Mental component scores. Note for Fig. 1a/b: SF-36 measures quality-of-life. The MCS of the SF-36 measures quality-of-life on four health domains: role limitations due to emotional problems, energy/fatigue, emotional well-being and social functioning. The PCS includes general health, physical functioning, role limitations due to physical health and pain. Scores range from 0 to 100, with higher scores indicating higher quality of life. Median scores are displayed as dots, with an interquartile range as lines, the corresponding values and significance can be found in Table 2. SF-36, 36-item Short Form Survey. PCS, physical component score. MCS, mental component score.
SF-36 Physical component scores. Note for Fig. 1a/b: SF-36 measures quality-of-life. The MCS of the SF-36 measures quality-of-life on four health domains: role limitations due to emotional problems, energy/fatigue, emotional well-being and social functioning. The PCS includes general health, physical functioning, role limitations due to physical health and pain. Scores range from 0 to 100, with higher scores indicating higher quality of life. Median scores are displayed as dots, with an interquartile range as lines, the corresponding values and significance can be found in Table 2. SF-36, 36-item Short Form Survey. PCS, physical component score. MCS, mental component score.
Three months after HBOT, out of 137 patients analyzed, 76 (56%) were responders, 43 (31%) were non-responder and 18 (13%) were negative-responders. Patient characteristics for each subgroup are shown in Table 3.
In the patients who received an extension to 50 or 60 sessions, median MCS changed from 39.3 (IQR 19.4–53.7) at baseline, to 46.8 (IQR 38.6–55.5) directly after HBOT, to 55.1 (40.6–64.1) at 3-month follow up (N = 23). For the PCS these scores were 27.5 (IQR 21.3–41.3), 32.5 (IQR 20.0–43.1), and 40.6 (IQR 26.3–48.1), respectively (N = 24). Wilcoxon signed rank indicated significant change in both MCS and PCS (for MCS: p = 0.006, Z= −2.8 directly after HBOT and p = 0.002, Z-3.0 at 3-month follow up, and for PCS: p = 0.016, Z= −2.4 and p = 0.012, Z= −2.5, respectively).
In the extension of treatment group, out of the 32 patients analyzed, 20 (63%) were responders, 6 (19%), were non-responders, and 6 (19%) were negative-responders. In the 105 patients analyzed in 40 sessions group this was 56 (53%), 37 (35%), and 12 (11%), respectively.
EQ-5D
The mean score on the visual analogue scale of the EQ-5D (EQ-5D VAS) improved from mean 37 (SD 14) at baseline to 46 (SD 20) directly after HBOT (p < 0.001), to 50 (SD 19) at 3-month follow up (p < 0.001), for 138 patients analyzed (Table 4).
And out of 163 patients analyzed, 99 (61%) improved more than the MCID (7.5 points) at 3-month follow-up, 16 (10%) patients had a deterioration of more than the MCID, and 48 patients (29%) did not improve or deteriorate more than the MCID.
Long COVID complaints questionnaire
Out of the 40 included complaints in the questionnaire, the complaints that were most often scored ‘severe to extreme’ at baseline were fatigue (87%), difficulty processing stimuli (80%), post-exertional malaise (75%), loss of physical fitness (71%) and concentration problems (68%). All symptoms and frequencies are shown in Figure A in the appendix.
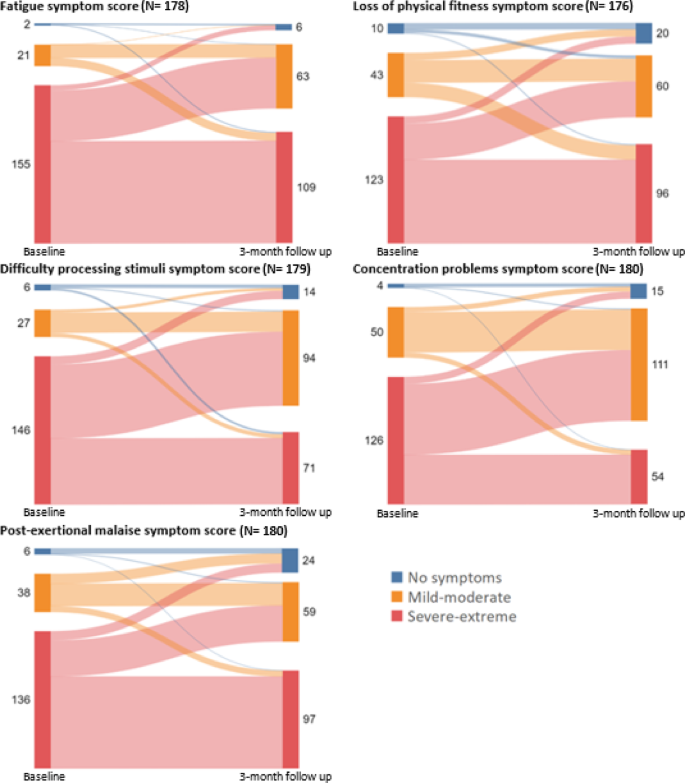
At 3-month follow up, for the top 5 symptoms there was a global decline in symptom burden, for example from severe-extreme symptoms to mild-moderate (Fig. 3).
For fatigue 55/155 (35%) patients with severe-extreme symptom score had less severe complaints at 3 month follow up. On the other hand, 9/21 (43%) patients with no or mild-moderate symptoms transitioned to severe-extreme complaints at 3-month follow up. Respectively, for difficulty processing stimuli 81/146 (55%) reported improvement and 6/33 (18%) deterioration, for post-exertional malaise 45/136 (33%) reported improvement and 6/44 (14%) deterioration, for loss of physical fitness 42/123 (34%) reported improvement and 15/53 (28%) deterioration and for concentration problems 77/126 (61%) reported improvement and 5/54 (9%) deterioration.
The most substantial decreases in symptom burden (from severe-extreme to less severe) were seen for word-finding problems (43/59 patients, 73%), irritability (44/61, 72%), memory problems (62/88, 70%), brain fog (70/103, 68%) and shortness of breath on exertion (38/68, 56%). All symptoms and frequencies over time are presented in Appendix Table C.
Absence from work
In the registry there were 214 people that were working before the onset of long COVID. Of these people, 105 (49%) were still able to work to a certain degree, and 91 people were completely unable to work due to complaints of long COVID (N = 214). Of the patients who were able to work, 94 (96%) had reduced their weekly working hours to a median of 12 (IQR 8–23) hours per week or 34% (IQR 22–60) of the hours stated in their contract (N = 98). Furthermore 78 (74%) working patients reported adjustments in the content of their work because of their illness (N = 102).
At 3-month follow up, 8 (11%) of patients who were not working at baseline due to long COVID were able to resume activities at work (N = 72). On average, they were able to work for a median of 9 (IQR 4–32) hours per week (N = 8).
Patients who were able to work at baseline but who had reduced their working hours because of long COVID, were not able to work more hours per week at 3-month follow up (median 12 (IQR 8–20), p 0.294). Content of work was no longer adjusted in 6 (9%) of patients (N = 68).
Adverse events
In the 232 patients who received HBOT there were 24 unsolicited adverse events. The most common unsolicited adverse event was barotrauma of the middle ear (11 patients). Furthermore, 2 patients had complaints of anxiety/claustrophobia during HBOT, and 1 patient had an episode with symptoms of shortness of breath. And, as stated before, 10 patients experienced worsening of fatigue or other long COVID symptoms during HBOT and terminated treatment before completion.
Solicited events during regular visits were fatigue (65%) and blurry vision (27%), which are common complaints associated with HBOT. These complaints were reversed at 3-month follow up, except for one patient who still experienced blurry vision. A consultation at the ophthalmologist revealed an incipient cataract, not requiring treatment at that time.