The study included 1253 VLBW infants: 727 during pre-implementation, 191 during post-implementation, and 335 during the sustainability period (Supplementary Table 1). Baseline characteristics were similar across cohorts. The proportion classified as low-risk was 41%, 44%, and 35% across the three periods.
Among low-risk infants, early antibiotic initiation decreased from 185/298 (62.1%) pre-implementation to 11/83 (13.3%) post-implementation and remained low in the sustainability period at 21/122 (17.2%), with no significant difference between post-implementation and sustainability (p = 0.4, Supplementary Table 2). For days 4–7, rates of blood culture collection, antibiotic initiation, bacteremia, and death or transfer were similar across periods. As rates of early antibiotic initiation among low-risk infants declined, the rate among high-risk infants was unchanged over the study period (Fig. 1).
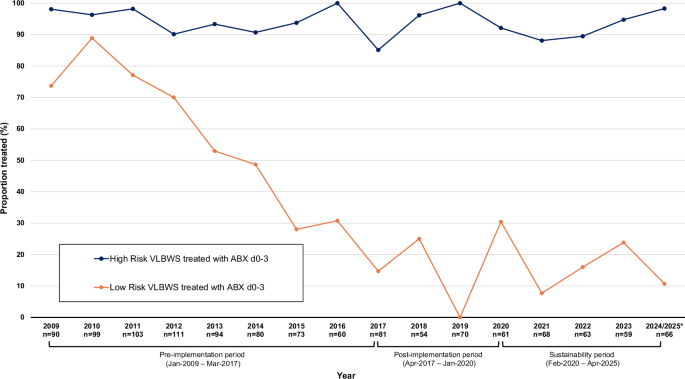
Annual proportions of very low birth weight (VLBW) infants receiving antibiotics on days 0–3 after birth from 2009 through April 2025 are shown by delivery risk category. The orange line represents low-risk infants (delivered by cesarean for maternal indications, without labor or rupture of membranes before delivery), and the blue line represents higher-risk infants. * Data for 2024–2025 were combined, as the sustainability period includes infants born through April 2025 only.
To assess whether changes were limited to low-risk infants or reflected broader practice shifts, we compared antibiotic use among all VLBW infants. Antibiotic initiation increased in the sustainability period compared to post-implementation (113/191 [59.2%] vs. 221/335 [66.0%], p = 0.04), though the proportion of low-risk infants was lower (43.5% vs. 36.4%, p = 0.05). During days 4–7, both antibiotic initiation (11.5% vs. 6%, p = 0.03) and blood culture collection (13.1% vs. 7.2%, p = 0.02) were lower in the sustainability period. Rates of death, transfer, and culture-confirmed EOS were similar across periods. Overall, 18/738 (2.4%) high-risk infants had culture-confirmed EOS, while no cases occurred among 488 low-risk infants (p
During the sustainability period, 21 low-risk infants (17.2%) received early antibiotics. Documented reasons included clinical change (n = 10), hypotension (n = 5), gastrointestinal pathology (n = 4), poor biophysical profile (n = 1), and hyperglycemia (n = 1).