Table 1 presents the basic socioeconomic characteristics of the households and respondents surveyed. A total of 3,889 individuals participated in the survey- 2,402 from the New Halfa and 1,587 from Nahr Atbara. Of these respondents, 45.6% were male and 54.4% were female, with a similar gender distribution in both locations. The overall average age of the respondents was 22.1 years. Specifically, the average age in New Halfa was 23.1 years, which is higher than in Nahr Atbara, where the average age was 20.7 years. For additional information about the region, including population size, latest year of MDA, and the number of primary health centers and health units, see Table S1.
The survey identified the occupation of the household head rather than the individual’s occupation, with farmers constituting the majority at 52.2%, followed by commercial skilled workers. New Halfa had a higher proportion of farmer households, while Nahr Atbara had a greater proportion of fishermen. The average annual household income across the study was 255,150 Sudanese pounds (approximately USD 438 as of January 31, 2023). However, households in Nahr Atbara reported a higher average income of 389,994 Sudanese pounds (USD 670) compared to those in New Halfa. The ownership rates for radios, refrigerators, and bicycles among the households were 42.2%, 23.6%, and 14.3%, respectively. Health insurance coverage was reported by 63.1% of all households, with 99.5% of these being publicly insured. Health insurance coverage was also higher in Nahr Atbra (72.7%) than in New Halfa (56.8%).
Table 2 presents data on each household’s access to water, sanitation, and excreta disposal. The questionnaire addresses household-specific issues regarding water and toilets, whereas questions about contact with water bodies are tailored to individuals. Among the total sample, 67.5% of households reported using packaged water, while 25.4% had piped water to the dwelling. In Nahr Atbara, 80.1% of households used packaged water, compared to only 59.2% in New Halfa. Meanwhile, approximately 34.8% of households in New Halfa reported having water piped into the dwelling.
In total, 70.7% of respondents reported having toilet facilities at home, with 72.7% in New Halfa and 67.7% in Nahr Atbara respectively. Regarding the type of toilet, pit latrine without slab was the most prevalent, accounting for 47.1%, followed by pit latrine with slab. Users of toilets that flushed into a septic tank or sewer pipe represented 8.3% and 3.4% of the total, respectively. Among the households without a toilet, about 20.1% used a neighbor’s facility, 2.1% used a communal toilet, and the remaining 77.9% engaged in open defecation. Of those practicing open defecation, 51.1% did so within 10 feet of their dwelling, while 48.4% did so at a distance greater than 10 feet. Open defecation in water bodies was less frequent. Approximately 55.1% of respondents urinated within 10 feet of their dwelling, with the figures being 62.4% in New Halfa and 44.6% in Nahr Atbara.
When individuals were asked if they came into contact with water bodies, an average of 84.1% confirmed that they did, with a slightly higher rate reported in Nahr Atbara. The primary reasons for water contact were leisure and swimming, accounting for 40.2% and 17.2% respectively. Farming and wading into the water were the next most common reasons, at 11.6% and 11.2% respectively.
Table 3 shows the survey results concerning disease-related behaviors, awareness, praziquantel usage, health facility utilization, and perceptions of community health workers. The responses regarding awareness and treatment represent one family member, while data on health utilization encompass all participants, including children. Regarding awareness, an average of 85.2% of respondents were familiar with schistosomiasis, and 94% accurately identified its source. Additionally, 64.1% of respondents could correctly recognize at least one symptom of the disease, and 64.4% were aware of the vector involved. However, only one out of 849 respondents correctly identified praziquantel as the appropriate medication.
The proportion of individuals who reported taking schistosomiasis treatment within the past six months was 35.2% overall, with the rate being approximately 3.7% higher in Nahr Atbara. Among the 134 respondents who had received medication, 85.1% obtained it through a community campaign, while 7.5% acquired it from a local pharmacy, and 3.7% received it at a health facility. The majority of respondents identified community health volunteers as the distributors of the medication, underscoring the significance of community campaigns as the primary source. Out of 840 respondents, each answering on behalf of their household, 87.4% experienced no difficulties in accessing praziquantel, whereas 12.6% faced challenges. Among those encountering difficulties, 62.6% attributed it to the unavailability of the drug in their town, and 27.1% cited its high cost.
Approximately 46.8% of respondents reported visiting a health facility in the past six months, with about 71.7% of those individuals visiting two or fewer times. Nearly 95.8% stated that the nearest health facility was within a 30-minute distance, and 56.5% were aware of their local health volunteer’s identity.
Prevalence
Figure 2 illustrates the estimated prevalence for each locality and village. The prevalence of S. mansoni in New Halfa and Nahr Atbara was notably high at 28.0% and 24.3%, respectively. Conversely, the prevalence of S. haematobium was relatively low-2.1% in New Halfa and none in Nahr Atbara. Figure 2 (c) and (d) detail the prevalence for individual villages. For S. mansoni, one village reported a peak prevalence of 68.2%. Among the 40 villages identified as high-endemic, 25 recorded prevalence exceeding 20%. In contrast, as shown in Fig. 2 (d), S. haematobium was found in a few villages in New Halfa, with two out of the 40 villages showing prevalence above 10%. (Refer to Table S2, Table S3 and Table S4 by villages and by socio economic factors, and Fig. S1 for heatmaps of S. mansoni and S. haematobium infection.)
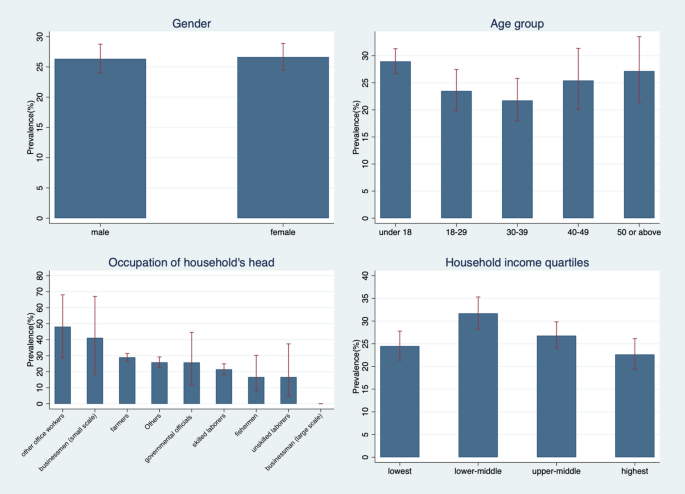
Figure 3 presents the prevalence by various socio-demographic characteristics. Among all respondents, no significant differences by gender in prevalence were observed. However, when examining prevalence by age group, some notable observations emerged. The prevalence in the under-18 age group was remarkably high, at 28.9%. In the age group of 20 and above, the prevalence remained 20%. This highlights the potential for significant prevalence in population groups beyond school-age children, particularly when exposure to infection is substantial and access to diagnosis and treatment is limited.
In the analysis of prevalence based on the occupation of each household head, families with office workers and small-scale business owners showed the highest prevalence, although the confidence intervals were wide. Households headed by farmers also showed a high prevalence, whereas those headed by fishermen had a relatively lower average prevalence. However, the confidence interval in this latter group was also broad.
In the few instances involving households of large-scale business owners, no infections were reported. Additionally, when analyzing household monthly income divided into quartiles, disparities between groups became apparent. The lower-middle income group exhibited the highest prevalence, in stark contrast to the highest-income group. Interestingly, the lowest income group, which one might assume to have poorer hygiene conditions, did not show the highest prevalence.
Infection and its associated factors
Among the total 2,941 individuals analyzed, 779 (26.5%) tested positive for S. mansoni, exhibiting a mean egg count of 116.71 eggs per gram (EPG) (Fig. 4). The highest count recorded was 1,776 eggs. As shown in Fig. 4, the distribution of egg counts among positive cases was right-skewed. For S. haematobium, a total of 2,870 individuals were analyzed, of which only 33, or 1.2%, tested positive. Of those who tested positive, egg counts ranged from 2 to 190, with an average of 18.6.
Table 4 presents the results of the double hurdle model used to examine the factors associated with S. mansoni infection status and infection intensity. The first hurdle applied a logit model, while the second hurdle used a zero-truncated negative binomial model. In the case of S. haematobium, we only report the results of the logit model, which is the first hurdle. The reason is that there were only 1.2% of positive cases, and there was an overfitting problem when applying the zero-truncated negative binomial model.
First, socio-economic conditions were associated with the likelihood of infection. Compared with individuals under 18 years of age, the likelihood of infection was significantly lower among adults. Specifically, the adjusted odds of infection were reduced for those aged 18–29 years (aOR = 0.70, p < 0.01), 30–39 years (aOR = 0.64, p < 0.01), and 40–49 years (aOR = 0.68, p < 0.05). However, this trend was not observed among individuals aged 50 years and older. Furthermore, when analyzing the second hurdle, which related to the intensity of infection, no significant age-related differences were observed.
Gender differences in the likelihood of S. mansoni infection were not observed. However, females showed marginally lower infection intensity (IRR = 0.84, p < 0.1). However, disparities in infection status were evident based on the occupation of the household head. Compared to farmers, households headed by unskilled laborers (IRR = 0.52, p < 0.05), skilled laborers (IRR = 0.57, p < 0.01), and fishermen (IRR = 0.50, p < 0.01) had significantly lower S. mansoni infection intensity. In contrast, household members from families headed by businessmen (aOR = 2.17, p < 0.01) and other office workers (aOR = 2.65, p < 0.05) had significantly higher likelihood of infection compared with those from farmer-headed households, though not higher intensity. There were no significant differences in infection probability or intensity related to income or assets. Similarly, no variations in infection status or intensity were associated with owning a toilet in the household.
One of the strongest predictors of S. mansoni infection was regular water contact. Individuals with regular water contact had a strongly higher likelihood of infection (aOR = 1.87, p < 0.01) and significantly greater intensity (IRR = 1.79, p < 0.01). Regarding water source, rainwater collection was associated with marginally higher likelihood of infection compared to having piped water into the dwelling (aOR = 11.11, p < 0.1) and significantly greater intensity (IRR = 1.72, p < 0.01). On the other hand, protected wells were linked to significantly lower infection intensity (IRR = 0.44, p < 0.01), and using packaged water was marginally associated with lower intensity (IRR = 0.81, p < 0.1). Protected springs were associated with marginally higher intensity (IRR = 1.44, p < 0.1).
Regarding the association between S. mansoni infection status and healthcare facility utilization, individuals residing within a 30-minute distance from healthcare facilities were less likely be infected (aOR = 0.57, p < 0.05), though no significant association was observed with infection intensity. Having visited a health facility in the past six months was marginally associated with lower infection likelihood (aOR = 0.81, p < 0.1), but not with intensity.
The last column of Table 4 presents the analysis results on S. haematobium infection and its associated factors. For S. haematobium infection, no significant differences by age or gender were observed. However, individuals from households headed by unskilled laborers had a significantly higher probability of infection (aOR = 7.09, p < 0.05). Likewise, households owning bicycles (aOR = 3.57, p < 0.05) were significantly more likely to be infected. Interestingly, water contact was not significantly associated with S. haematobium infection. However, use of rainwater as the primary source was strongly associated with higher infection probability (aOR = 48.18, p < 0.01) Although there were notable variations in infection intensity among different groups, the small sample size in the model (N = 33) makes it difficult to draw meaningful conclusions from these differences.
Table 5 presents the associations between S. mansoni infection status, praziquantel consumption, and awareness of schistosomiasis. The analysis was limited to primary household respondents (N = 556) who provided information on praziquantel use in the past six months and their awareness of schistosomiasis, rather than including the entire sample. Therefore, Table 5 results separately from Table 4, although the same model was used in Table 4.
The participants who reported taking praziquantel within past six months exhibited a slightly lower probability of infection than those who did not take the medication. However, this difference was not statistically significant (aOR = 0.91, p = 0.66). Additionally, no statistically significant differences were found when investigating the impact of accurate knowledge about the disease’s source, vector, symptoms, and preferred treatment on the probability of infection. Nevertheless, individuals who accurately identified at least one symptom demonstrated significantly lower infection intensity than those who did not. Conversely, the group that correctly identified the medication showed higher infection intensity. This finding, however, may not be meaningful due to the very small number of individuals (N = 1) who provided correct answers about the medication.
Figure 5 illustrates the S. haematobium egg count. The left graph includes zero observations, whereas the right graph displays only the distribution of positive cases. Out of the total 2,870 samples, a vast majority, 98.85%, tested negative. The mean prevalence was 2.16%, with the maximum egg count observed being 190.